Stroke in Women & Men : Understanding the Signs and Symptoms
what are the symptoms of a stroke in a woman or in a man?
Stroke is a medical emergency that can have a devastating effect on the life of a woman. It is important to recognize the symptoms of stroke in women as early as possible to reduce its long-term effects. The most common signs and symptoms of stroke in women include sudden numbness or weakness on one side of the body, confusion, difficulty speaking or understanding speech, vision problems, dizziness, and severe headache. Other signs may include difficulty walking, loss of balance or coordination, and changes in mood or behavior. If you experience any of these symptoms it is important to seek medical attention immediately.
Strokes are one of the leading causes of death and disability worldwide. Knowing the FAST face, arm, speech, time (FAST) acronym can help you recognize the signs and symptoms of a stroke quickly.

FAST stands for
Face drop,
Arm weakness,
Speech slurred and
Time to call emergency number.
If you spot any of these symptoms in someone, it is important to act quickly and call an emergency number as soon as possible. This will ensure that the person receives timely medical attention which can significantly reduce their risk of disability or death from a stroke.

With my patient Nilayatakshi Iyer - Stroke Rehabilitation
Types of stroke
Mini strokes, also known as transient ischemic attacks (TIAs), are a type of stroke that affects women more than men. They often have a sudden onset and can last from several minutes to 24 hours. While mini strokes may not cause permanent damage, they can still be dangerous and should be taken seriously. What are the symptoms of a stroke in a woman, a mini stroke? It is important for women to be aware of the signs and symptoms associated with mini strokes so they can seek medical attention as soon as possible if they experience any of them. In this article, we will discuss the common symptoms of mini strokes in women, how to recognize them, and when to seek medical help.
Common mini stroke symptoms in a woman or man include sudden numbness or weakness in your face, arm, or leg; confusion; difficulty speaking or understanding speech; loss of balance or coordination; and vision changes. If you experience any of these symptoms, it’s important to get medical help immediately as this could be an indication that you are having a mini stroke.
Ischemic Stroke
Ischemic stroke is a type of stroke that occurs when the blood supply to a part of the brain is blocked or reduced. It is the most common type of stroke, accounting for about 87% of all cases. It can be caused by a number of different factors, including high blood pressure, atherosclerosis, diabetes, and smoking. Ischemic strokes can have serious consequences and can lead to long-term disability or even death if not treated promptly and properly. Symptoms may include sudden numbness or weakness on one side of the body, confusion, trouble speaking or understanding speech, vision problems, dizziness, and difficulty walking. Treatment for an ischemic stroke may include medications to dissolve clots or reduce swelling in the brain as well as lifestyle changes such as eating a healthy diet and exercising regularly.
A. Thrombotic stroke
Thrombotic strokes are one of the most common types of stroke and can be caused by a blood clot obstructing an artery in the brain. The clot can be formed due to a variety of factors, such as high cholesterol levels, diabetes, smoking, or even a genetic predisposition. Symptoms of thrombotic stroke include sudden weakness or numbness on one side of the body, confusion and difficulty speaking or understanding speech, and severe headaches. Treatment for thrombotic strokes includes medications to dissolve the clot, surgery to remove it, and lifestyle changes to reduce your risk for future strokes, and physiotherapy.
B. Embolic stroke
Embolic stroke is a type of stroke caused by an obstruction in the blood vessel. This can happen when a piece of plaque, fat, or air bubbles travel through the bloodstream and get stuck in a blood vessel in the brain. When this happens, it can block off the flow of oxygen and nutrients that are needed for normal brain functioning. As a result, embolic strokes can cause serious damage to the brain and even death if not treated quickly. The symptoms of embolic stroke include sudden weakness or numbness on one side of the body, confusion or trouble speaking, vision problems, dizziness or loss of balance, and severe headache. Treatment for embolic stroke includes anticoagulants to prevent further clotting and medications to reduce swelling around the affected area. In some cases surgery may be necessary to remove any obstructions from the blood vessels as well.
Hemorrhagic Stroke
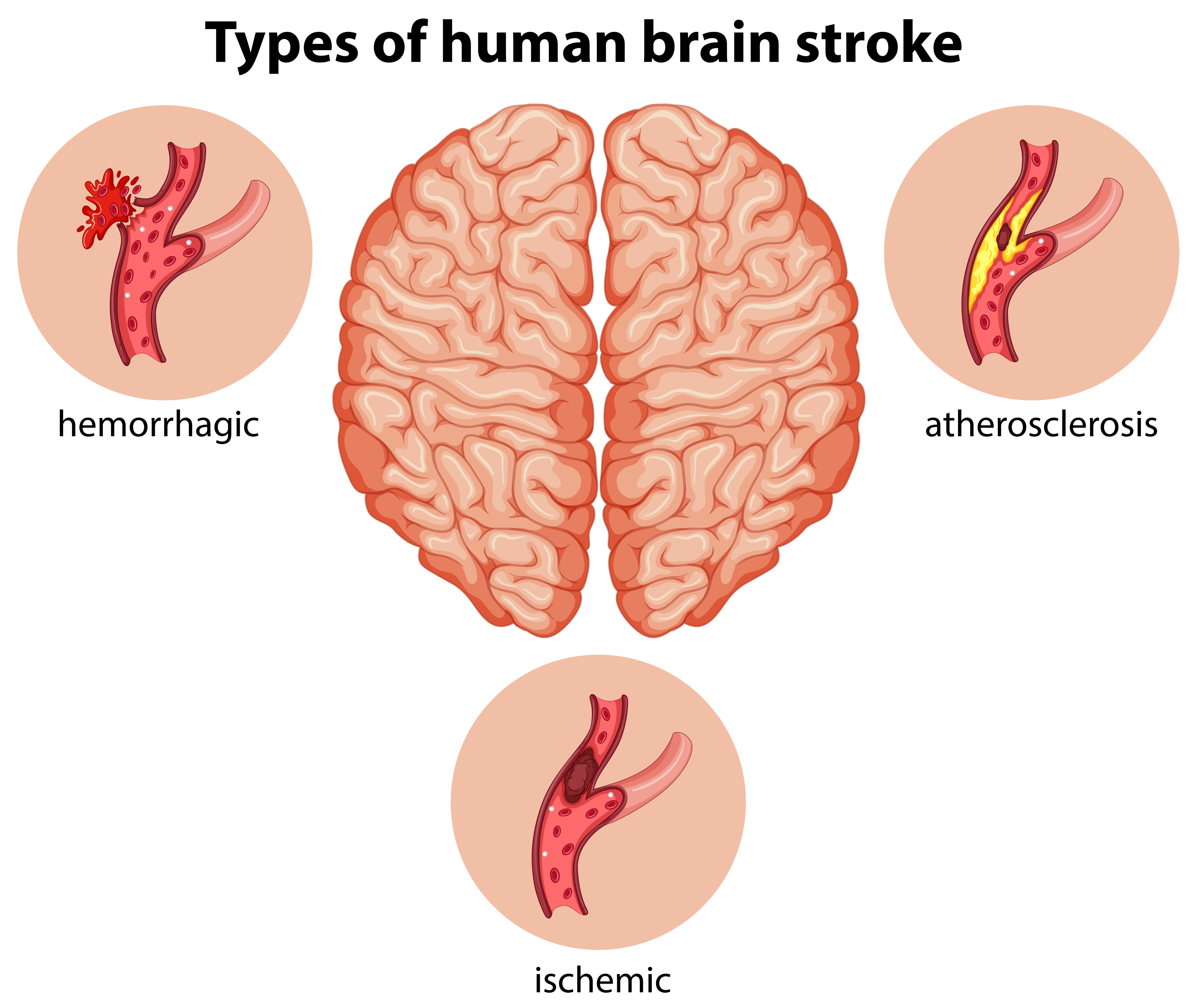
Hemorrhagic stroke is a type of stroke that occurs when a weakened blood vessel ruptures and bleeds into the surrounding brain tissue. It is one of the most serious types of strokes, as it can cause permanent damage or even death if not treated quickly. The risk factors for hemorrhagic stroke include high blood pressure, smoking, alcohol use, and certain medications. Early recognition and treatment are key to reducing the risk of long-term disability or death from this condition.
A. Intracerebral hemorrhage
Intracerebral hemorrhage (ICH) is a type of stroke that occurs when a blood vessel in the brain ruptures and causes bleeding within the brain tissue. It is one of the most serious forms of stroke and can result in long-term disability or death. It is important to be aware of the risk factors, signs, and symptoms of ICH so that prompt medical attention can be sought if necessary. Early diagnosis and treatment are essential for reducing the risk of complications from ICH and improving patient outcomes.
B. Subarachonoid hemorrhage
Subarachnoid hemorrhage (SAH) is a type of stroke that occurs when an artery in the brain ruptures and bleeds into the space between the brain and its protective covering, known as the subarachnoid space. It is a life-threatening condition that can result in significant neurological damage or death if not treated quickly. SAH is most commonly caused by aneurysms, which are weakened areas of blood vessels in the brain that can burst and cause bleeding. Other causes include head trauma, arteriovenous malformations (AVMs), or certain medical conditions such as vasculitis. Treatment for SAH includes medications to reduce swelling, surgery to repair or remove damaged arteries, or endovascular treatments like stenting or embolization.
What is recurrent stroke?
Recurrent strokes are strokes that occur more than once in a person’s life. They can be caused by the same underlying condition or a different one. People who have experienced a stroke are at higher risk of having another one, and the risk increases with each successive stroke. Understanding the causes and risk factors of recurrent strokes is essential to reducing their occurrence and improving patient outcomes. This article will explore the causes, risk factors, and treatment options for strokes.
Causes of stroke
Stroke is an event caused by a disruption in the blood supply to the brain, either due to a blockage or a rupture in an artery. This interruption of blood flow can cause brain cells to die, resulting in stroke-related disabilities and even death. Knowing the causes of stroke can help people take preventive measures and reduce their risk of having one. Common causes of stroke include high blood pressure, smoking, diabetes, physical inactivity, unhealthy diet, alcohol consumption and family history. It is important to be aware of these risk factors so that they can be addressed before it’s too late.
Common risk factors
Stroke is a medical condition that can have serious, long-term consequences. It is important to understand the risk factors associated with stroke in order to reduce the likelihood of experiencing one. The most common risk factors for stroke, including age, lifestyle choices, and underlying health conditions. Understanding these factors can help you make informed decisions about your health and take steps to reduce your risk of stroke.

Stroke is a medical condition that can have a significant impact on an individual’s life. Fortunately, there are risk factors that can be identified and addressed to reduce the likelihood of having a stroke. Age, lifestyle choices, and underlying health all play a role in increasing the risk of stroke. As age increases, so does the risk of stroke. Lifestyle choices such as smoking, drinking alcohol, and eating unhealthy foods can also increase the chance of having a stroke. Additionally, underlying health conditions such as high blood pressure or diabetes can increase the probability of having a stroke. It is important to be aware of these risk factors for stroke so that preventative measures may be taken to reduce them. By understanding how age, lifestyle choices, and underlying health all contribute to stroke risk it is possible to take steps towards reducing this risk and living healthier lives.
Major Risk Factors
High blood pressure.
Heart disease.
Diabetes.
Smoking.
Birth control pills (oral contraceptives)
History of TIAs (transient ischemic attacks).
High red blood cell count.
High blood cholesterol and lipids.
Lack of exercise
Obesity
Excessive alcohol use.
Other risk factors
Older age. > 55,
Race.
Gender. men>women
History of prior stroke.
Heredity or genetics.
Complications
Stroke is a serious medical condition that can have life-altering consequences. It occurs when the blood supply to part of the brain is interrupted or reduced, depriving the brain of oxygen and nutrients. As a result, cells in the affected area begin to die and can cause permanent damage. Stroke can cause physical, cognitive, and emotional complications that can significantly impact a person’s quality of life. These complications include paralysis, difficulty speaking or understanding language, memory loss, depression and anxiety. With early detection and proper treatment, many of these complications can be minimised or prevented.

Physiotherapy
Stroke is a life-altering event that can cause physical, cognitive, and emotional difficulties. Physical therapy can be an important part of the recovery process for stroke patients. It helps to restore movement and strength as well as improve balance, coordination, and range of motion. Physical therapy can also help to reduce pain and spasticity while improving overall quality of life. Through careful assessment, personalized treatment plans, and skilled instruction in therapeutic exercises, physical therapists work with stroke patients to maximize their functional abilities.
Physiotherapy plays a vital role in helping women who have suffered from stroke to regain their function and mobility. Physiotherapists work with women stroke survivors to reduce the risk of further disability, improve their ability to move, and help them return to their daily activities. The main goals of physiotherapy in stroke cases are to reduce pain, improve muscle strength and coordination, increase range of motion, improve balance and gait, and promote independence in daily activities. Physiotherapists also provide education on how to prevent further strokes and how to manage any residual impairments. By providing these services, physiotherapists can help stroke survivors achieve the best possible outcome.
Physiotherapy Goals
Acute Care
Aims :
1) Prevent recurrent stroke
2) Monitor all vitals, dysphasia adequate nutrition, bowel & bladder function.
3) Prevent any complications
4) Mobilize the patient
5) Encourage resumption of self-care activities
6) Provide emotional support & education for patient & family
7)Screen for rehabilitation and choice of settings
Rehabilitation care
Aims :
1) Set physical therapy rehabilitation goals; develop rehabilitation plan and monitor the progress of the condition.
2) Manage sensory-motor deficits
3) Improve functional mobility & independence
4) Prevent & treat complications
5) Monitor functional health conditions
6) Discharge planning (safe residence recommendation, patient & care givers education & continuity of care)
7) Community – reintegration
Community care
Aims :
1) Assist patient to reintegrate into community
2) Enhance family and caregivers functioning
3) Co-ordinate continuity of patient care
4) Promote health and safety and prevent further hospitalization
5) Advice properly on community supports, valued activities and vocational reintegrate

Physiotherapy Techniques
Stroke is a major cause of disability in women and men those who are suffering and physical therapy interventions can help improve motor control. Neurofacilitatory techniques such as Bobath, Rood, Brunnstorm and PNF are used to improve motor control in stroke patients. These techniques involve re-educating the nervous system to activate muscles that have been affected by the stroke. Through these techniques, the patient can regain their ability to move, balance and coordinate their movements. Physical therapists use these techniques to help stroke patients regain normal movement patterns and improve their overall quality of life.
What are the symptoms of a stroke in a woman? Physical therapy
Physical therapy interventions to improve the symptoms of stroke in men & women.
A. To improve motor control
1.Neuro Facilatory techniques like
a. Bobath
Stroke is a leading cause of disability worldwide, and it affects motor control. Fortunately, there are various neurofacilatory techniques that can help improve motor control in stroke patients. One such technique is Bobath, which is based on the idea that the nervous system can be retrained to regain lost function after a stroke. The Bobath approach focuses on restoring normal movement patterns and improving coordination, balance and strength through specific exercises and activities tailored to the individual's needs. It also helps to reduce spasticity (abnormal muscle tightness) and pain associated with stroke-related impairments. By using this approach, stroke patients can regain their independence and improve their quality of life.
b. Rood
Stroke is a debilitating condition that can cause severe motor and sensory deficits. Fortunately, there are treatments available to help improve motor control in stroke patients. One such treatment is Rood, a neurofacilatory technique that has shown promising results in improving motor control in stroke patients. This technique works by stimulating the nervous system with electrical signals to facilitate movement of the affected area. It also helps to reduce spasticity and improve strength and coordination in the affected limbs. Rood has been used successfully in many clinical settings, and it has been found to be an effective treatment for stroke-related motor deficits. With its non-invasive approach, Rood is a safe and effective way to improve motor control in stroke patients, allowing them to regain their independence and quality of life.
c. Brunnstorm
Stroke is a leading cause of disability and can be debilitating for those who suffer from it. Fortunately, there are ways to improve motor control in stroke patients with the use of neurofacilitatory techniques like Brunnstorm. This technique involves the use of specific exercises that help to strengthen weakened muscles and improve coordination, balance, and posture. It also helps to reduce spasticity and increase range of motion. By improving motor control in stroke patients, Brunnstorm can help them regain their independence and quality of life.
d. PNF
Stroke is one of the leading causes of disability in the world and can lead to motor control impairments. To improve motor control in stroke patients, physical therapists are increasingly turning to Proprioceptive Neuromuscular Facilitation (PNF) techniques. PNF is a form of physical therapy that uses specific movements and positions to stimulate muscles, increase range of motion, and improve coordination. By using PNF techniques, physical therapists can help stroke patients regain their motor control and improve their quality of life.
2. Learning therapy approach
a. Conductive education
Conductive education is an effective approach to help stroke survivors improve their motor control and functional abilities. It is a holistic approach that combines physical, cognitive, and educational components to increase the patient’s level of independence. The primary goal of conductive education is to enable stroke survivors to regain control over their movements and activities of daily living. This therapy focuses on teaching them how to use their remaining motor skills in order to perform everyday tasks such as dressing, eating, and walking. Conductive education also helps stroke survivors develop problem-solving skills and strategies for dealing with any physical or cognitive limitations they may have.
b. Motor learning theory
Motor learning theory is a scientific approach to understanding how humans learn and control motor skills. It provides a framework for understanding the process of motor skill acquisition and its application to physical therapy and rehabilitation. Motor learning theory has been used to develop various therapies for stroke patients, such as learning therapy approaches. These approaches focus on using repetition and practice to increase the patient's ability to perform previously learned tasks, as well as introducing new tasks that can be used in everyday life. By focusing on motor control in stroke patients, these therapies have been shown to improve functional outcomes and quality of life following a stroke.
3. Functional electrical stimulation (FES)
4. Biofeedback
#Hemiplegic shoulder pain management
Hemiplegic shoulder pain is a common problem for people with hemiplegia, a condition caused by stroke or other neurological disorder. To manage this type of pain, it is essential to use the right physiotherapy techniques. Exercises, functional electrical stimulation, repositioning and proper handling are all methods that can be used to help reduce the discomfort associated with hemiplegic shoulder pain. By using these techniques in combination, it is possible to improve range of motion and strength in the affected area while also helping to reduce pain levels. With proper management and treatment, individuals can regain their quality of life and return to their normal activities.
1.Exercise:
Hemiplegic shoulder management is an important part of rehabilitation for those who have suffered a stroke. It involves active weight bearing exercise, grading tactile, proprioceptive, and kinesthetic stimulation to reduce edema and spasticity. By actively engaging in these exercises, the patient can improve their range of motion and strength while reducing pain associated with the condition. Through a combination of these treatments, hemiplegic shoulder management can help improve quality of life for those affected by this condition.
2.Functional electrical stimulation:
Functional electrical stimulation (FES) is an emerging therapy for hemiplegic shoulder management. It has been used to treat patients with neurological conditions such as stroke and cerebral palsy, and is showing promise in treating those with hemiplegia. FES works by using electrical currents to stimulate the muscles, allowing them to contract and relax in a coordinated fashion. This can help improve range of motion, strength, and coordination of the affected arm. By providing targeted stimulation to specific muscles, FES can also reduce spasticity and pain associated with hemiplegia. With proper use of FES, patients can regain control over their affected arm, allowing them to perform daily activities more easily and independently.
3.Passive limb physiotherapy:
Stroke is one of the leading causes of long-term disability and hemiplegic shoulder management is an important part of stroke rehabilitation. Passive limb physiotherapy is an effective way to manage the shoulder pain and stiffness caused by a stroke. It helps to reduce muscle spasms, improve range of motion, and reduce pain. It also helps to improve functional ability in daily activities such as dressing, bathing, and eating. Passive limb physiotherapy can be used in combination with other treatments such as exercise therapy or electrical stimulation for better results. This article will discuss how passive limb physiotherapy can be used to effectively manage hemiplegic shoulder pain in stroke patients.
4.Position and proper handling:
Stroke is a leading cause of disability in the world, and hemiplegic shoulder management is a critical part of stroke rehabilitation. Proper positioning of the affected arm and proper handling can help reduce the risk of shoulder pain and other complications associated with stroke. By using specific postures, exercises, and other techniques, healthcare professionals can help patients manage their hemiplegic shoulder pain more effectively. In this article, we will discuss the importance of position and proper handling in hemiplegic shoulder management for stroke patients.
5.Neuro facilitation:
Hemiplegic shoulder pain is a common complication of stroke. It can have a significant impact on the health and quality of life of stroke survivors. Neuro facilitation is an effective approach to managing this condition, as it involves exercises that help to improve the mobility and strength of affected muscles. Neuro facilitation also helps to reduce pain and improve range of motion in the shoulder joint, which can help prevent further sablucsation or disability. This article will discuss the role of neuro facilitation in hemiplegic shoulder management following a stroke, as well as its potential use cases and benefits.
6.Pain relief physiotherapy and sling:
Hemiplegic shoulder pain is a common complication after stroke and can have a significant impact on quality of life. Pain relief physiotherapy, reciprocal pulley, and sling are three different strategies for managing hemiplegic shoulder pain that can be used in combination or separately. Pain relief physiotherapy can help reduce the amount of pain experienced by while sling is a mechanical devices that can be used to provide support to the affected arm. By combining these different strategies, it is possible to manage hemiplegic shoulder pain in an effective and efficient way.
7.Reciprocal pulley
#Limb physiotherapy
#Chest Physiotherapy
#Position
Stroke is a serious medical condition that can lead to permanent disability or even death. The proper positioning of the body during a stroke can have a significant impact on the outcome of the stroke, as it can help to reduce reflex-inhibitory patterns. Proper positioning during a stroke can help to reduce reflex-inhibitory patterns and improve recovery outcomes. Physiotherapist also provide some tips and advice on what positions are best for stroke patients.
#Tone management
Muscular tone management is an important part of managing stroke patients. It helps to restore the patient's normal range of motion, reduce pain and improve their quality of life.
#Sensory re-education
After a stroke, sensory reeducation is essential to help the patient regain their ability to feel and control their body. Sensory reeducation helps to retrain the brain and nervous system by providing sensory input in a controlled environment. This helps the patient relearn how to interpret sensations from their body parts, as well as how to move those parts of the body in a coordinated manner. Through this process, patients can regain sensation, movement and coordination that had been lost due to the stroke.
#Balance training
Balance training is an important part of rehabilitation for people who have experienced a stroke. It is essential for helping them regain their balance and mobility, as well as reducing the risk of falls. With the right balance training program, stroke survivors can improve their quality of life and reduce their risk of further injury. In this article, we will discuss the importance of balance training after a stroke and how to do it safely and effectively.
#Fall prevention
Falls are one of the most common and serious consequences of stroke. To reduce the risk of falls, it is important to incorporate balance training into your post-stroke recovery plan. Balance training can help improve coordination, strength, and confidence while also reducing the risk of falls. By incorporating balance training into your recovery plan, you will be able to regain independence and confidence while also reducing your risk of falling. This article will provide you with tips on how to do fall prevention after stroke through balance training.
#Gait re-education training
Gait re-education is an important part of rehabilitation after stroke. It helps people to regain their ability to walk safely and independently. Balance training is an important component of gait re-education, as it helps to improve balance, coordination and stability while walking. Balance training can be done in a variety of ways, such as using balance boards or exercise balls, or by doing specific exercises that focus on improving balance and stability. It is important to work with a physical therapist or other medical professional when doing gait re-education after stroke so that you can get the most out of your therapy sessions. Gait re-education is an important part of stroke rehabilitation. It helps to improve the patient's ability to walk and move again after a stroke. Gait training involves exercises that focus on strengthening the muscles and improving balance, coordination, and range of motion. It also helps to improve walking speed, endurance, and overall quality of life. There are several different types of gait re-education that can be used depending on the patient's needs. This article will discuss how to do gait re-education after stroke and what exercises should be included in a gait training program.
#Functional mobility training
Functional mobility training is an important part of stroke rehabilitation. After a stroke, individuals often experience reduced mobility and strength. Functional mobility training helps to restore the ability to move around independently and safely, which can improve quality of life for stroke survivors. Functional mobility training involves a variety of exercises that target specific muscles and joints affected by the stroke. These exercises can help increase strength, balance, coordination, and range of motion in order to improve functional abilities such as walking and transferring from one surface to another. By engaging in functional mobility training after a stroke, individuals can regain the ability to perform activities of daily living with increased independence. This type of rehabilitation is essential for improving quality of life for those who have experienced a stroke.
#Upper limb physiotherapy
After stroke, in upper limb physiotherapy, certain techniques can help patients to regain the use of their affected limb. Different techniques like constrained induced therapy, functional electrical stimulation and electromyographic biofeedback are used to facilitate recovery. These techniques can be used to improve range of motion, strength, coordination and dexterity in the affected limb. They also help reduce spasticity and pain in the affected area. Furthermore, these techniques can be used in combination with other rehabilitation strategies such as occupational therapy, physical therapy and speech therapy for a more comprehensive approach to recovery.
1. Facilitation models:
Stroke is one of the leading causes of disability in adults and can cause significant impairments in movement, sensation, and coordination. To improve upper limb function after stroke, a range of facilitation models have been developed to support rehabilitation. These models are based on evidence-based principles of motor learning and can be used to guide the delivery of therapy interventions. They focus on task-specific practice, providing feedback to the patient on their performance, and using repetition to promote motor learning. By utilizing these facilitation models, therapists can help individuals with stroke regain their upper limb function.
2. Constrained induced therapy:
Constrained induced therapy for upper limb after stroke is a novel form of physical therapy that has been gaining traction in recent years. This therapy involves the use of physical restraints to limit the movement of the affected limb, while encouraging increased use of the unaffected limb. By doing so, it helps to promote motor recovery and improve the patient's quality of life. The goal is to help those who have suffered from a stroke regain some level of independence and function in their daily lives. This therapy has been used successfully in numerous clinical studies, with promising results for patients who have undergone this type of treatment.
3. EMG:
Electromyographic biofeedback (EMG) is an important tool in the rehabilitation of upper limb function after stroke. EMG biofeedback helps individuals to consciously control their muscles and can be used to improve movement accuracy, strength and coordination. It also provides information to therapists about muscle activity during movement, which can be used to design more effective rehabilitation programs. This article will discuss the application of EMG biofeedback for upper limb after stroke and its potential benefits for patients.
4. FES:
Functional electrical stimulation (FES) is a promising new treatment for upper limb function after stroke. FES involves the use of electrical current to stimulate the muscles of the affected arm, allowing them to contract and relax in a coordinated manner. This can help improve range of motion, strength and coordination in the affected arm. FES has been shown to increase independence and reduce disability in those with upper limb impairments due to stroke. It can also help reduce spasticity, which can lead to improved quality of life for those with stroke-related impairments.
Prevention: Tips to avoid brain stroke
Brain stroke is a serious condition that can lead to long-term disability or death. To prevent brain stroke, it is important to take preventive measures such as:
1.eating a healthy diet,
2.exercising regularly, and
3.avoiding smoking.
Additionally, controlling risk factors such as:
1.high blood pressure and
2.diabetes can help reduce the risk of brain stroke.
It is also important to be aware of the signs and symptoms of brain stroke so that medical attention can be sought immediately if needed. Taking these steps can help individuals protect their health and reduce their risk for brain stroke.

Conclusion
Stroke is a life-threatening medical emergency that affects both men and women. It is important to know the symptoms of a stroke in a woman so that timely intervention can be done for the best possible outcome. The most common symptoms of a stroke in a woman are sudden numbness or weakness, confusion, difficulty speaking or understanding, loss of balance or coordination, and severe headache. Pro Physiotherapy Clinic provides comprehensive at-home physical therapy services for stroke rehabilitation. Our team has experienced physical therapists who specialize in helping people recover from a stroke through evidence-based therapeutic exercises and activities that help improve mobility, strength and balance. We also provide customized treatment plans to ensure the best possible outcome for our clients. With our at-home service, we make sure that our patients get the right care they need without having to leave their homes.
Hope you liked this article, to read the similar article click the 🔗 Squeeze Ball Exercises for Stroke Patients – I Need a Squeeze Ball.

